Benjamin Franklin once said there are only two things certain in life: death and taxes. Fast-forward 225+ years, north of the 49th parallel. Another charismatic leader, Justin Trudeau, head of the Liberal Party of Canada, proclaimed another certainty: no Liberal member of Parliament will ever vote against “a woman’s right to choose” on his watch.
Now, you can bet the ranch the newly minted 23rd Prime Minister of Canada will keep this promise. Nothing stirs fear in the hearts of fence-sitting politicians like the “A” word. No one even says that word out loud, at least not in polite circles. So, the likelihood of any political debate ensuing around that issue is pure fantasy.
But, what if we flipped the coin and made the conversation about something else? What if the focus was on supporting a woman’s choice to continue her pregnancy, especially in difficult circumstances? What if we were to have a robust public conversation about ways to create a context of “real choice” for women to have children and raise them under optimal circumstances?
Now, this would be a conversation worth having, one that is arguably long overdue. However, even where there is agreement about the merits of proactive prenatal support, not everyone agrees about how best to serve women during their pregnancies, or even on the need for a continuum of support for mother and child after birth.
The problem is that choice – in the abstract – is a fallacy. Legal equality didn’t level the playing field between men and women, bringing about effective equality of opportunity and outcomes (or so the argument goes). All women don’t have the same advantages or disadvantages, either. Pregnancy undeniably alters a woman’s body, though, bringing about life-shifting changes. This last factor, especially, ought to be given weight in any real discussion about women’s reproductive choices, but it usually isn’t.
Yet people who are acting out of a genuine concern for expectant mothers ought to be able to agree on certain things, such as that it makes sense to provide optimal health care, as well as access to the necessities of life, for women who are expecting and that the maternal rights of pregnant women must be respected, precisely because they are bringing the next generation of citizens into the world.
It should be obvious that women who are carrying a child need to be free from extraordinary pressures. Less obvious, unfortunately, is the need for a policy of zero tolerance for any form of violence, or coercion, toward them at this time of heightened vulnerability.
There is a new concept taking root in the area of maternal-child health care. It’s called “social maternal health care.” Programs incorporating this new approach are available only to a small number of women right now. However, this evolving model is nonetheless shaping the discussion of how best to support the maternity needs of all women.
In Montreal, a team of doctors, educators, social workers, midwives and therapists is combining their skills to help women and children in situations of vulnerability. To do so, they are bringing the health care system’s resources under one roof, an approach they like to refer to as supporting “fragile nests.”
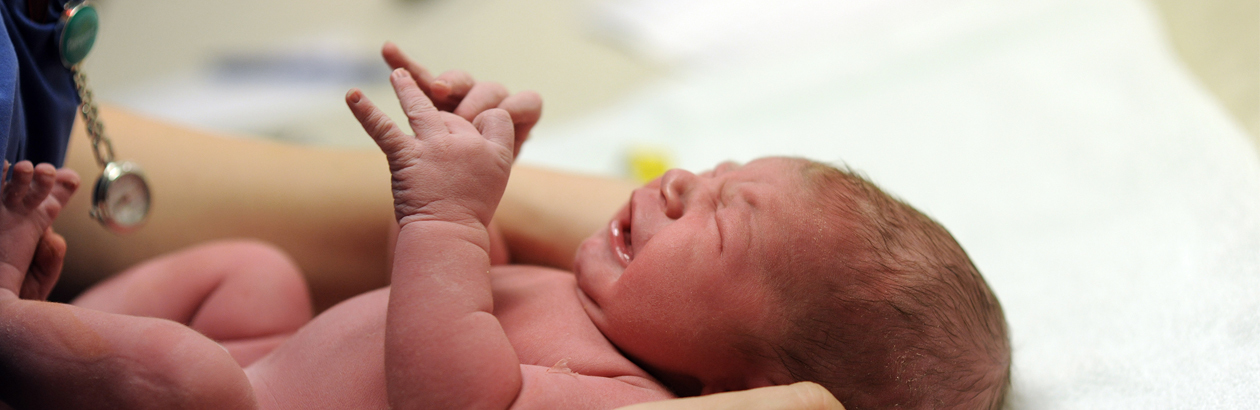
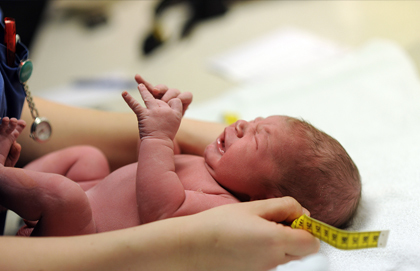
La Maison Bleue is a maternal-child health care centre where dedicated professionals work alongside volunteers in a collaborative spirit to support women when they need it most: during pregnancy, at childbirth, in the critical postpartum period and beyond. They do so by providing comprehensive maternal-infant health care, with follow-up care for the entire family, all in one package.
La Maison Bleue was founded in 2007 by Dr. Vania Jimenez, a birthing family doctor affiliated with McGill University and Montreal’s Jewish General Hospital, along with her daughter Amélie Sigouin, its general director. The centre’s mandate incorporates best practices in early childhood development in its holistic vision of maternal-child care.
Jimenez laughs when she recalls how they came up with the name for the centre: “It was my daughter’s idea. Blue is her favourite colour. Her wedding was blue-themed. Blue is also the colour of a water bubble, so it fits with pregnancy. [It’s about] enveloping families,” she says.
“We wanted to bring it together under one roof,” Jimenez says of the neighbourhood hubs – there are two “Blue Houses” – that provide maternal health care and other services to women and their families. The notion of “one roof” cuts both ways: La Maison Bleue is a human space anchored in a worldview weaving threads on the village theme, where people come together to help one another. The women who come to this multi-faceted maternal resource centre may learn about it by word of mouth or through the Internet. In some cases, they are referred by health and social service agencies.
Pascale Rolland, La Maison Bleue’s communications director, is quick to point out that the centre is bilingual: services are offered in English as well as French. She says the centre is in the process of putting together a better English website before launching into a broader discussion of what La Maison Bleue is all about.
However, it soon becomes clear that the “A” word is on Rolland's mind. After initially waxing euphoric about the “miracle stories” of the women who come through the maternity centre’s doors for birthing care, unprompted, she nervously says, “We are pro-choice. We respect women’s choices.”
Later, Jimenez is taken aback when she hears about her colleague’s remarks. “Yes, we are a full-service health centre,” she says, cautious of making any misstep, “but the women who come here have kept their pregnancies. They are late-term.”
The centre’s houses are located in very different neighbourhoods. One is in Montreal’s fabled Park Extension, with its deep roots in the Greek community. The other, nestled in the Côte-des-Neiges area on the western slope of Mount Royal, is in one of the most diverse neighbourhoods in Canada, home to more than 100 different ethnic groups. Plans for a network of Blue Houses that will bring together a whole range of services for mothers and their babies are in the works.
The Park Ex location is in Justin Trudeau’s riding of Papineau, which might account for Rolland’s pro forma statement about choice. Trudeau has promised to donate his family’s Universal Child Care Benefit (UCCB) to La Maison Bleue. Public support for any new social program is always fragile; and not unlike many other innovative projects, this maternal health-care initiative is made possible by a private-public partnership.
All medical services are delivered under the auspices of public health care, while everything else is gratis, courtesy of private donors. Now, clearly, the centre won’t be depending on Trudeau’s personal UCCB contribution to stay afloat. But, the Prime Minister’s opinion carries weight, especially in his own riding, where a thumbs-up (or down) can make or break a project.
Jimenez, who insists she is a huge supporter of the public system, is grateful just the same for the non-profit model that allows the centre to fundraise for vulnerable women and their families, many of whom are immigrants or refugees.
As might be expected, patients at the two locations have somewhat different needs. In the more established Park Ex neighbourhood, there are far fewer single mothers. The Côte-des-Neiges area has always had higher crime rates than average. This means more stress for families at the margins of society. Inevitably, each of the Blue Houses takes on “the colour of the neighbourhood,” Jimenez says.
Demographic considerations aside, “the hybrid model allows us to multiply the efficiencies of the public sector,” she says. This is all to the good. As health care now stands, doctors may include maternal care in their practices, but it’s not obligatory. And it’s not the rule. Jimenez dreams that one day, though, this will become the norm. “If we could extend this approach to the whole world, that would be great; but it’s not realistic.”
It stands to reason that if mothers are the principle caregivers of the family, then the family’s health is about as good as mom’s. In a bygone era, when there was a new baby on the way, the woman was often described as being “in the family way” – quaint phrasing by today’s standards. But this simple language belies an intuitive recognition that motherhood and family life are intimately intertwined. So, there is a definite argument for making maternal health care the linchpin of family health care.
Present health-care realities aside, Jimenez is confident that La Maison Bleue’s model of proactive support of mothers and children who are at risk “is changing the trajectory by providing massive support to one per cent of the population that uses a lot of the health resources.” Most of all, she is proud of the fact that “none of the patients pay a cent.”
La Maison Bleue’s annual report for 2014-2015 showed that it followed 186 women during their pregnancies, assessing and monitoring their physical and mental health before and after childbirth. Expectant mothers – those lucky enough to benefit from its full-service approach – have the choice of a physician or midwife to attend their deliveries and are followed by a nurse at all times. The centre also provides postpartum care for the new mother and her baby, with home visits in the first few days after childbirth. These continue later at one of the Blue Houses.
Baby boomers may recall stories of a time when the nurses from the Victorian Order of Nurses paid home visits to their own mothers. However, the practice gradually disappeared, along with any postpartum care for the mother as maternal-infant health care was subsumed under the mantle of public health care. Hence the need for a revitalized approach to maternal-infant health care.
Care for the entire family is an important axis of service for La Maison Bleue’s patients. Its recent report shows that it followed 602 families, 913 children and 159 partners, for a total of 1,673 people in one year.
However, the centre’s program goes well beyond the recreational activities associated with events for Mom & Tots. After an initial assessment of the family’s needs (with the family), the professional staff comes up with an intervention plan to address various problems experienced by family members. Depending on the family’s needs, this might involve referrals to other government agencies in the areas of employment, education, housing, immigration and youth protection.
While some of the centre’s patients are simply poor people who need a hand up, others have greater challenges such as mental health problems, disability and substance dependence. Then there are the victims/survivors of violence and abuse, for whom pregnancy is doubly difficult. Some of these women (and youths) may be trying to exit prostitution or get out of an abusive relationship. For some who arrive at La Maison Bleue’s doors, continuing their pregnancies is a true act of bravery. These are women (and young girls) who have been raped by soldiers, making it necessary for them to leave their countries of origin, where rape victims are often blamed and targeted for reprisals.
La Maison Bleue also provides care for fathers, often neglected in the rush to help mothers and children in situations of vulnerability. “We have to take care of the dad,” Jimenez says. “He’s often the one who is taking care of mom when she has problems. So he becomes our patient, too.” These fathers, many of them newcomers to Canada, are often facing additional pressures associated with intercultural integration post-migration. Finding one’s place in a new country is never an easy task, but it’s all the more difficult with a new baby on the way in an economic downturn.
Ever the optimist, the physician-literary author – Jimenez’s most recent novel, Je suis une pierre brûlant (I Am a Burning Stone), based loosely on her experience working in an Inuit community in northern Quebec – says that it is precisely in these areas of crisis intervention “where we can have the biggest impact.”
In Canada, of course, there is no legal protection for a woman who wants to carry her pregnancy to term and no sanctions against those who take it away from her.
It’s great to include dads in the process of caring for pregnant women. But, what happens when dad doesn’t want a baby in the picture? Things can get very scary and ugly for women and their dependent children.
Loss of pregnancy, resulting from assault, isn’t a factor in determining the severity of a crime. The former Conservative Government promised to bring in legislation that would make pregnancy a factor in sentencing, but somewhere between the Senate scandals and myriad Tory troubles, the idea failed to gel and no bill was ever tabled.
It is, however, against the law to fire a woman for being pregnant; nevertheless, women are put out of their homes for this very reason all the time. In a country that prides itself on being fair and inclusive, it’s open season on expectant mothers.
Brian Jenkins, who works for Campagne Québec-Vie / Quebec Life Coalition, a pro-life organization, is all too aware of these facts. This is why he is setting up a centre to aid women who are expecting a baby. “We saw the need for a centre to help pregnant women,” he says. Last summer, the organization received a flurry of calls from women who were being pressured to leave their homes by reluctant fathers unhappy about the news that a new baby was on the way.
The calls were in response to a new website he had just set up (in French only), Enceinte et Inquiète? (Pregnant and Worried?). Pregnant women were fleeing under “threat of violence,” he says. So, the soft-spoken 55-year-old man began reaching out to anyone he thought might help create a “safe space” for them.
Jenkins contacted various people to find suitable lodgings. He finally reached a pastor in a trendy, predominantly French-speaking district known as The Plateau – on the eastern flank of the mountain – who offered to convert the upstairs rectory of l’église Saint-Enfant-Jésus du Mile-End into a safe haven for women and children in need of immediate assistance.
So far, there are plans for 10 emergency spaces at the rectory. Since December, a team of volunteers has been busy getting the premises in shape for the new arrivals, cleaning, plastering, painting and refurbishing the old quarters to make them family-friendly.
But what happens to expectant women in urgent need of an escape route in the meantime?
Jenkins recounts the plight of a mother-to-be, already with two kids, who contacted him. She was fleeing an abusive relationship. The problem was, she lived on the South Shore of the Greater Montreal region and couldn’t make the journey into town to get the help she needed. “They need money and a vehicle,” he says, matter-of-factly.
All he can do in such cases is put women in touch with social service agencies in their municipality, say a prayer and hope for the best. Shelters are overcrowded, waiting lists for subsidized housing long, and the health care system, overtaxed and underfunded – to meet real needs on the ground. Still, he maintains a fragile hope that things will get better. “The plan is to start small and grow the project,” he says.
Like many pro-lifers, Jenkins has a faith-based perspective that guides his actions. He believes God is calling him to do this work. He got involved in the movement 15 years ago when some friends approached him to raise money.
But, lately he’s felt an inner urging to be more present in the lives of women who are in need – precisely because they are carrying a new life – by helping them in a hands-on way. “I see pregnant women being pressured during a period in their lives when they need rest, and I am trying to provide a restful environment for them,” he says.
Unlike some pro-lifers, and some of their prochoice opponents, Jenkins doesn’t trade in inflammatory rhetoric. His unassuming demeanour itself has a calming effect. The language he uses is spiritual and ecological. “God is the source of life, and love, who sustains life,” he says. “I just wish society could have more respect for gestating life.”
Margaret Somerville, the founder of the Centre for Medicine, Ethics and Law, who holds the Samuel Gale Chair in Law at McGill University, has long been an advocate for an informed-consent process in decisions regarding pregnancy, often referenced to health issues. More recently, though, the author of Bird on an Ethics Wire: Battles about Values in the Culture Wars has put the accent on social support for pregnant women. She says this must include “support to go through with a pregnancy.”
It is a striking irony that at a juncture in history when we understand more than ever before about the complexity and fragility of the symbiotic relationship between mother and child, beginning before birth, that maternal-infant health care isn’t the first priority of the health care system. This raises the question of what it will take to move maternalchild care onto the public agenda as part of a real world vision for Canada in the 21st century.